DENIAL MANAGEMENT
Services
Boost your revenue collection by identifying and overturning underpayments and wrongful claim denials. Several factors have impacted the revenue generation tendency of the laboratories including; ICD-10 implementation, DRG shifts. Also, legal reforms like the re-implementation of local and national coverage determination (LCDs and NCDs) when combined with increased payer requirements_ uplifted a nationwide trend of increasing claim denials.
We help practitioners to combat all of these challenges and step towards greater productivity and elevate the scalability of their business. Since our team of experts safeguards your medical billing system from claim denials and rejections. In this way, we make sure that every single dollar you deserve just lands in your accounts and nowhere else.
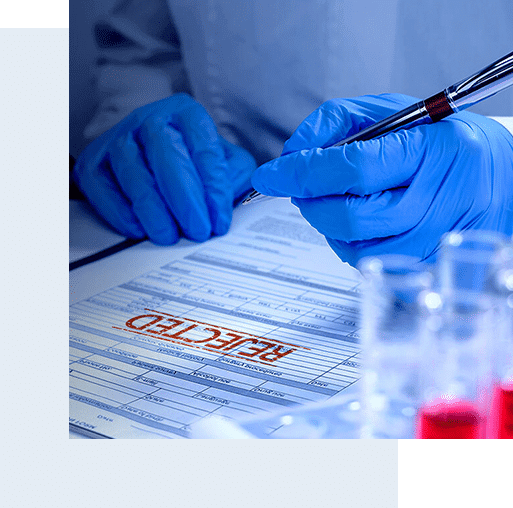
Ensure Safety Of Your Claims & Revenue!
We address your claims’ eligibility issues upfront in order to appeal for your reimbursements in time. So you don’t have to compromise over your earnings anymore. It is our responsibility to protect your medical billing system from such errors that cause claim denials and we are experts in our business. Improve the revenue flow across your accounts with reliable claim denial management services.
STRATEGIES TO PREVENT MEDICAL CLAIMS DENIAL
Maintain
Workload On Practitioners
Claim denials impose an increasing workload on practitioners in order to trace, rectify, and resubmit the denied claims. The dilemma became clearer when it was revealed that most of the healthcare organizations never addressed these claim denials.
Climbing denial rates is significantly hurting the bottom line for several healthcare professionals all around the country. With great expertise, our dedicated team of certified medical billers provides efficient claim denial management services to generate better outcomes.


Have a
Primary Objective
It is the primary goal of our denial management experts to resolve underpayments while reducing regulatory risks to keep your financial performance optimum. Partner with us to acquire intelligent solutions for denial management in order to break new grounds. Our vision for smart denial management services is to help healthcare providers become highly efficient at saving their practice from further revenue loss.
- Save Revenue Loss.
- Reliable Support.
- Reduce risk.
We help practitioners to recover their millions of outstanding dollars and manage their medical business with innovative solutions. Find an advanced, innovative, and reliable support to achieve your financial goals and advance your journey to the future of success.

Provide
Efficient Billing Services
We provide all-in-one denial management solution with deeper insights to identify and mitigate the reasons to reduce claim denial rates. We help your organization to meet its financial goals.
Our dedicated team would ensure steady cash flow and profitable revenue cycle management with reliable denial management services. Our claim denial management services include analyzing, identifying, and resolving key problems that obstacle claim success rate. We classify those problems on cause & source and align our Lab Billing Services in the direction of mutual business success.
Improved
Cash Flow
Enhance your clean-claims rate, maximize reimbursements, and prevent revenue loss with reliable and proficient assistance in handling the appeals. We aggressively follow-up with each claim, mitigate the causes of denials and improve cash flow. If claims are not followed rigorously then a huge amount of revenue is lost between the cracks.
Therefore, we engage with your claim submission process from information collection to reimbursement of your services. We streamline your medical billing operations for faster appeals and improved cash flow while lowering the cost of managing denied claims and the administrative burden. Do more with less stress!
What Strategies do we use to
Improve your Medical Business

Sophisticated
Rules Engine
We define advance payer rule engines to prepare reimbursable claims, catch the denial activity, and comply with federal regulations. In this way, we leave no room for those issues that could become a reason for claim denials.

Clean
Claims
It is one of the highest priorities of our organization to increase the clean claim rate for your practice. So we can reduce the transactional complexity of your lab business & help you build a profound relationship with insurance payers.

In-Depth
Analytics
Our experts track down the preparation cycle of a claim to identify from start to reimbursement collection. Our goal is to eradicate the cause of claim denial. Also, we ensure 100% accuracy throughout the billing cycle.
Automated Appeal
Management
Our automatic solutions for lab billing enable us to process manual appeals management processes faster and ensure a seamless workflow for effective denial management. In this way, our solutions allow you to collect maximum reimbursements.

Medical Clearing
House Solutions
Before submitting the electronic claims to payers, our experts scrub the claims for any missing data to validate the claims against payer-specific rules. Hence, we always make sure that your claims get paid every time.

Recover
Every Dollar
If you’re worried that you’ve lost a significant amount of money due to claim denials in the past. Then relieve your stress now. Our experts aggressively follow-up on your payments to make sure that you can get paid completely.
Learn how we support your business growth by offering a choice of preconfigured Lab Billing Services. We design lab revenue cycle management services in order to meet the financial needs of your business. Contact us to schedule a free demo of the most reliable and highly promising healthcare revenue cycle management services for your medical lab.

