
Are you facing delays in patient care & inefficient workflows? Prior authorization management is growing heavier day by day due to a huge administrative burden. It has become a cumbersome process filled with manual tasks and roadblocks that dilute the original intent. However, it was created to improve safety, streamline workflows, ensure care standards continuity, and regulate costs. A medical practitioner must understand that it is an important part of healthcare revenue cycle management. Handling it properly is the key to the success of healthcare organizations. The prior authorization process involves an illustration of a PA form to an insurance firm by a healthcare provider for identifying why a specific medicine or procedure prescribed is essential. In this blog, I will highlight the importance/need of the PA process and ways to manage it effectively.
What Is Prior Authorization?
Healthcare providers need a signoff that will ensure that a specific process is already covered for a patient. Even before the patient qualifies for coverage or insurance agencies agree to pay for medical procedures and medications, etc. This whole process is commonly referred to as precerts and is also known as pre-certification or (PA) prior authorization.
Significance Of PA In RCM
Non-approval after treatment can lead to a huge bill either for a healthcare provider or patients that are the reason PA is crucial in revenue cycle management. Though, it takes a lot of valuable time for medical practitioners whose main goal is to provide quality healthcare services to the patients. So, errors in prior authorization not only affect patient care but also cripples the RCM function.
The Pre-Certification Process
- Why do you have to wait so long to get the approval for the necessary procedure? After treatment non-approval can cost a huge bill either for a provider or a patient.
- Healthcare providers have to contact the payers regarding the approval process of necessary procedures when an insurance company doesn’t approve certain medical equipment or treatments.
- For instance, a cardiologist may prescribe a CT scan to a patient, but it may have already been recommended by a pulmonologist two weeks before for the same patient. The insurance agency will not pass the particular healthcare process unless there is a need for an additional scan and it is clear that the past scan has already been reviewed.
- In addition to this, it is highly important to ensure that the information supporting the medical necessity claim is accurate and true. Administrative staff will sometimes begin documentation by evaluating PA rules manually for the particular coverage plan linked with the patient because healthcare and clinical billing systems are rarely integrated
- A provider’s administrative staff may be referencing out-of-date rules as they change frequently. Within a specified payer, it is not uncommon for the rules to even differ from health plan to health plan as they are not standardized.
- The provider can submit the claim to the insurance payer after confirming that prior authorization is not required. But that does not mean the claim will be approved significantly.
- Once the payer confirms authorization is needed, it will require to get a number assigned by the insurance carrier that corresponds to the request of the PA. In addition to this, the required CPT codes for the particular procedure are needed to track down and include when the final claim is submitted.
- Until the resolution of the pre-certification request_ a denial, redirection, or approval, it is the responsibility of healthcare providers to keep a follow-up with the insurance agency. This part of the process can lead to significant wasted effort or time as it is often improvised and restructured.
Topmost Advantages Of Prior Authorization
- Identify whether the recurrent and ongoing service is worthwhile for the care of patients.
- Ensure that the drug or service is truly medically necessary that is requested by the physicians.
- Manage the possibility of overprescribing and help in controlling costs.
- Make sure services are not duplicated in cases where patients are dealing with multiple specialties.
How Long Does A PA Take To Approve? Depending on requirements stipulated by the payer, the level of manual work, and the complexity of PA requests, it can take a day to a month to process. The delay can cause problems for both patients and healthcare providers. Moreover, obstacles like postponement decline the patient’s adherence to treatment and medication. Taking professional support and utilizing advanced lab billing solutions may help to reduce the amount of time a pre-certification takes. So, you would be able to keep a very strict follow-up schedule and know when the first request was sent. This helps you to prevent the dreaded delay that is typically caused by prior authorization. The Bitter Truth The inability of advanced tools to reconcile the incomprehensible variables of health plans having pending request PA forms creates significant technology gaps. As the below-mentioned graph depicts
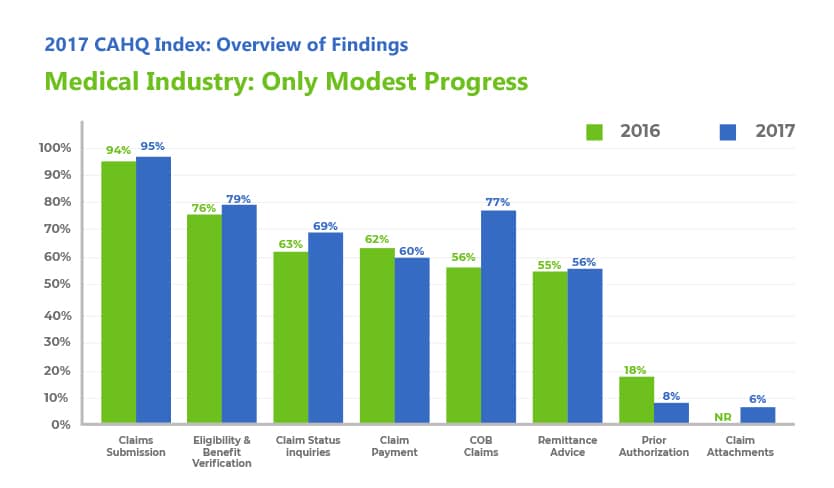
This graph shows past industry-wide adoption rates of the 2017 CAQH index. Though 70% e-prescribing, 87% of physicians with primary care have adopted EHR, 92% of PA is being done manually and 8% utilize digital PA. What we seem to have is a gap on the part of the insurance industry rather than a technology gap. How to bridge the technology gap let’s look at proactive ways to handle PA in the revenue cycle management.


